Healthcare professions stand distinct for their intrinsic value derived from a steadfast commitment to patient-centred care. The ethos that drives these professions is deeply rooted in the understanding and respect for the individual needs, experiences, and dignity of each patient. This approach forms the cornerstone of quality healthcare, ensuring that the treatment and care provided are tailored to meet the unique requirements of patients. As society grapples with complex health challenges and evolving patient expectations, the relevance and importance of healthcare professions have never been more pronounced. Through a detailed exploration of what patient-centred care entails, its significance, and its implementation, this article sheds light on the inherent value of healthcare professions and underscores why they are indispensable to the well-being of our communities.
The Core of Patient-Centred Care: Explaining the Fundamentals
Patient-centred care is a holistic approach that places the patient at the heart of healthcare delivery. It is characterised by a respectful and responsive attitude towards individual patient preferences, needs, and values, ensuring that patient values guide all clinical decisions. At its core, patient-centred care encompasses several key elements: respect for patients’ values, preferences, and expressed needs; coordination and integration of care; information, communication, and education; physical comfort; emotional support and alleviation of fear and anxiety; involvement of family and friends; and continuity and transition. This approach contrasts sharply with traditional models of care, which often prioritise efficiency and standardisation over the individual needs of the patient. By focusing on the patient as an individual rather than a mere recipient of care, healthcare professionals can create a more satisfying and effective healthcare experience for both patients and themselves.
Empathy and Compassion: The Intangible Skills of Healthcare Workers
Empathy and compassion represent the heart and soul of patient-centred care. These intangible skills go beyond the technical competencies required in healthcare professions, touching on the ability of healthcare workers to connect with patients on a personal level. Empathy involves understanding the patient’s situation, feelings, and concerns from their perspective and communicating this understanding back to the patient. Compassion extends this by actively seeking to alleviate the patient’s suffering through attentive care and supportive actions. These qualities are critical in building trust and rapport between healthcare providers and patients, facilitating open communication, and ensuring that care is aligned with the patient’s needs and wishes. The cultivation of empathy and compassion in healthcare settings not only enhances patient satisfaction and outcomes but also contributes to the professional satisfaction and resilience of healthcare workers, highlighting their central role in the delivery of effective patient-centred care.
Healthcare Innovations and Patient-Centred Approaches
The integration of innovative technologies and methodologies into healthcare has significantly enhanced the ability to provide patient-centred care. Innovations such as electronic health records (EHRs), telemedicine, and personalised medicine are transforming the way healthcare is delivered, making it more accessible, efficient, and tailored to individual patient needs.
EHRs facilitate seamless communication and information sharing among different healthcare providers, ensuring that a patient’s care team is fully informed of their health history, preferences, and needs. Telemedicine extends the reach of patient-centred care by allowing patients to receive consultations and follow-up care from the comfort of their homes, thus removing geographical and physical barriers to care. Personalised medicine, leveraging advancements in genomics and biotechnology, offers treatments and interventions that are specifically designed to align with an individual’s genetic makeup, significantly improving the efficacy of medical interventions. These innovations underscore the shift towards healthcare systems that prioritise patient engagement, autonomy, and personalised care, reflecting a deeper understanding of the value of treating patients as active participants in their healthcare journey.
Education and Training for Patient-Centred Care
The shift towards patient-centred care necessitates a corresponding evolution in the education and training of healthcare professionals. Courses and programmes, particularly those focusing on an MSc in healthcare management, are increasingly incorporating patient-centred care principles into their curricula. These healthcare management courses aim to equip future healthcare leaders with the knowledge and skills to implement effective patient-centred practices within their organisations. Such programmes cover a broad range of topics, including ethical considerations in patient care, communication strategies, leadership in healthcare settings, and the integration of technology in patient-centred solutions. A master’s in healthcare management emphasises the importance of empathy, ethical patient interaction, and the management of healthcare teams in a way that prioritises patient needs and outcomes. Graduates of these programmes are prepared to navigate the complexities of healthcare management and champion patient-centred approaches in their practices.
This focus on education and training ensures that the next generation of healthcare professionals is well-equipped to maintain and enhance the intrinsic value of healthcare professions through dedicated, compassionate, and patient-focused care.
Challenges in Delivering Patient-Centred Care
Delivering patient-centred care is not without its challenges, which stem from both systemic and operational barriers within healthcare systems. One significant challenge is the often-limited resources available to healthcare providers, including time constraints, staffing shortages, and financial limitations. These constraints can hinder the ability of healthcare professionals to spend adequate time with patients, tailor care plans to individual needs, and provide the level of emotional support that patient-centred care requires. Furthermore, the existing healthcare infrastructure and payment systems may not always support or incentivise patient-centred practices, instead favouring efficiency and volume of care over quality and personalisation. Additionally, there’s the challenge of ensuring that all members of a diverse healthcare team, including doctors, nurses, and support staff, are fully committed to, and trained in patient-centred principles. Overcoming these challenges requires changes at the institutional and policy level and a cultural shift within healthcare organisations towards valuing and prioritising patient-centred care.
The Impact of Patient-Centred Care on Health Outcomes
The adoption of patient-centred care has a profound impact on health outcomes, significantly contributing to improved patient satisfaction, better patient engagement, and enhanced quality of care. By focusing on the needs and preferences of patients, healthcare providers can develop care plans that are more likely to be followed by patients, leading to improved adherence to treatments and medications. This active involvement of patients in their care not only empowers them but also leads to more informed decision-making, resulting in care that is more effective and aligned with patient goals. Moreover, by addressing the emotional and psychological needs of patients, patient-centred care can improve the overall patient experience, leading to higher levels of patient satisfaction and trust in the healthcare system.
Conclusion
In conclusion, the essence of patient-centred care lies in its unwavering commitment to treating patients with dignity, respect, and empathy, ensuring that healthcare services are tailored to meet the unique needs and preferences of individuals. The shift towards patient-centred approaches in healthcare is not just a philosophical ideal but a practical necessity that has shown tangible benefits in terms of improved health outcomes, patient satisfaction, and the efficient use of healthcare resources. However, the journey towards fully realising the potential of patient-centred care is fraught with challenges, including systemic barriers, resource limitations, and the need for a cultural shift within healthcare organisations.
The role of education and continuous professional development, especially through courses focusing on healthcare management, is critical in equipping healthcare professionals with the skills and knowledge necessary to navigate these challenges and implement effective patient-centred care. As healthcare continues to evolve, the dedication to patient-centred principles will undoubtedly play a central role in shaping the future of healthcare delivery. Embracing patient-centred care is not only inherently valuable for healthcare professions but is also essential for building a healthcare system that is responsive, equitable, and capable of meeting the diverse needs of the population it serves.
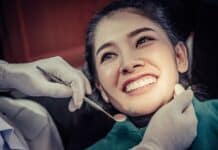
Image by DC Studio on Freepik